The big question is pretty simple: is it tonsillitis or strep throat? The answer, however, can get a little confusing.
Here's the key difference you need to remember: strep throat is a specific bacterial infection that causes tonsillitis, but most of the time, tonsillitis is actually caused by a virus. Even though the symptoms can feel exactly the same, figuring out whether it's viral or bacterial is the single most important factor for your treatment plan.
Getting to the Core of the Problem
When a brutal sore throat hits, knowing what's behind it is the first step toward feeling better. People often use "tonsillitis" and "strep throat" like they're the same thing, but they're not. Tonsillitis is just the general inflammation of your tonsils—those two lumps of tissue at the back of your throat. Think of it as a symptom, not a specific sickness.
Strep throat, on the other hand, is a specific infection caused by bacteria called Group A Streptococcus. This bacteria goes right for the throat and tonsils, causing a pretty severe case of bacterial tonsillitis. But here's the catch: most cases of tonsillitis aren't caused by strep. They're caused by the same viruses that give you a common cold or the flu.
This distinction is everything when it comes to treatment.
- Viral Tonsillitis: Antibiotics won't do a thing. Treatment is all about supportive care—rest, fluids, and pain relief—while your body's immune system does the heavy lifting.
- Strep Throat (Bacterial Tonsillitis): This absolutely requires antibiotics. The medicine is crucial for knocking out the bacteria, preventing serious complications, and stopping you from spreading it to others.
Because the symptoms overlap so much, just looking in the mirror isn't enough to tell what's going on. A proper medical diagnosis, which usually means a quick throat swab, is the only way to know for sure. Understanding this relationship helps explain why one sore throat gets better with tea and rest, while another needs a doctor's visit and a prescription.
Key Takeaway: Think of tonsillitis as the "what" (your tonsils are inflamed) and the cause (viral or bacterial) as the "why." Strep throat is just one very specific—and very important—"why" that demands targeted medical treatment.
Quick Guide: Tonsillitis vs. Strep Throat
To cut through the confusion, this simple table breaks down the essential differences between general tonsillitis and the specific bacterial infection we call strep throat.
| Feature | Tonsillitis (Usually Viral) | Strep Throat (Bacterial) |
|---|---|---|
| Primary Cause | Various viruses (e.g., cold, flu) | Group A Streptococcus bacteria |
| Key Symptoms | Gradual onset, cough, runny nose | Sudden, severe pain, fever, no cough |
| Standard Treatment | Supportive care (rest, fluids, pain relief) | Antibiotics (e.g., penicillin, amoxicillin) |
This at-a-glance comparison makes it easier to see why getting the right diagnosis is so critical for getting the right care.
The Real Culprit: Viral vs. Bacterial Invaders
To really get to the bottom of the tonsillitis vs. strep throat debate, you have to look past the symptoms and pinpoint the microscopic invader causing all the trouble. The most critical difference isn't what your throat looks like—it's whether the cause is a virus or a bacteria. It's a classic battle between two totally different types of germs.
Think of tonsillitis as a descriptive term, not a specific illness. It just means your tonsils are inflamed. Most of the time, this inflammation is the result of a viral attack from the same culprits behind the common cold or flu, like rhinovirus or adenovirus. Sometimes, it’s even the Epstein-Barr virus, which is famous for causing mono.
Strep throat, on the other hand, is a very specific infection. It’s caused by one—and only one—type of bacterium: Group A Streptococcus (GAS). This isn't a broad category of germs; it's a single, targeted bacterial assault on your throat and tonsils.
Why the Cause Dictates the Cure
Figuring out whether the invader is viral or bacterial is the single most important step because it completely changes the game plan for treatment. Viral infections just have to run their course; your immune system is already equipped to fight them off over time. Antibiotics, which are designed to kill bacteria, are totally useless against viruses.
Bacterial infections like strep throat are a different story. They need a targeted antibiotic treatment to wipe out the bacteria for good. Without that intervention, the bacteria can hang around and lead to serious health problems down the road.
Key Insight: A quick peek at your throat often isn't enough to tell a viral infection from a bacterial one. Since the treatments are worlds apart, the only way to be sure you're fighting the infection correctly is to get a diagnostic test, like a rapid strep test or a throat culture.
The Global Impact of a Single Bacterium
While most cases of tonsillitis are relatively mild viral issues, the specific bacterial infection of strep throat has a massive impact worldwide. Globally, there are over 600 million cases of sore throats caused by GAS each year. In the U.S. alone, that adds up to 5.2 million outpatient visits annually for people under 65. The stakes are especially high for kids, with an estimated 288.6 million episodes of Strep A sore throat hitting children aged 5-14 every year. You can learn more about the global burden of Group A Strep and see just how critical an accurate diagnosis is.
Untreated strep isn't just a lingering sore throat; it poses a risk of severe, long-term complications. These can include rheumatic heart disease, which contributes to over 300,000 deaths worldwide every year. This data really drives home why identifying and treating this specific bacterial invader is a global health priority.
This distinction is crucial:
- Viral Tonsillitis: Your body's immune system is the main line of defense. Treatment is all about supportive care—managing the pain and fever while your body does the heavy lifting to clear the virus.
- Strep Throat: Your body needs backup. Antibiotics are essential to kill the bacteria, which not only helps you feel better faster but also prevents the infection from spreading and causing severe issues like rheumatic fever or kidney inflammation.
A Detailed Symptom Showdown: Telltale Signs to Watch For
When you're dealing with a raw, painful throat, every swallow can feel like an ordeal. While both viral tonsillitis and strep throat cause serious discomfort, their symptom profiles often have subtle but critical clues that point to the root cause. Learning to spot these differences is the first step in figuring out what to do next.
The real goal here is to tell the difference between a viral infection that will likely go away on its own and a bacterial one that needs a doctor's attention. Paying close attention to how your symptoms unfold can give you a pretty good idea of what you're up against before you even make a call.
The Onset and Severity of Pain
One of the biggest clues in the tonsillitis vs. strep throat puzzle is how fast the pain shows up and how bad it gets. The timeline itself offers major hints.
A viral sore throat usually creeps up on you. It might start as a mild scratchiness that gets worse over a couple of days. The pain is annoying, for sure, but it’s often manageable.
Strep throat, on the other hand, is known for its dramatic entrance. The pain often comes on suddenly and intensely, going from zero to excruciating in less than 24 hours. People often describe it as feeling like swallowing glass.
The All-Important Cough
While many symptoms can overlap, the presence or absence of a cough is a huge differentiator. It’s one of the clearest signs that can help you lean toward a viral or bacterial cause.
If your sore throat comes with a nagging cough, a runny nose, or sneezing, you're almost certainly dealing with a virus. These are the classic calling cards of the common cold and flu, which happen to be the most frequent culprits behind tonsillitis.
Key Differentiator: A cough is a strong signal of a viral infection. The Group A Streptococcus bacteria responsible for strep throat don’t typically cause respiratory symptoms like coughing or congestion. The infection is almost entirely focused on your throat and tonsils.
Taking a Look at Your Throat and Tonsils
A quick peek in the mirror can reveal some visual clues, but remember that this isn't a substitute for a real diagnosis. Both conditions will cause red, swollen tonsils, but there are a few specific signs that scream strep.
- White Patches or Pus: While you can see white spots with both, prominent white streaks of pus coating swollen, fiery-red tonsils are classic signs of strep.
- Petechiae on the Palate: Look for tiny red dots (known as petechiae) on the roof of your mouth. This is a very characteristic sign of a strep infection and is rarely seen with viral tonsillitis.
- "Strawberry Tongue": In some cases, strep can make the tongue look red and bumpy, another sign that points away from a simple virus.
Understanding the different signs of a sore throat can help you describe your symptoms more clearly to a doctor.
To make things clearer, let's break down the common symptoms in a side-by-side comparison.
Symptom Analysis: Viral Tonsillitis vs. Bacterial Strep Throat
This table breaks down the key symptoms to help you spot the differences between a viral and a bacterial throat infection.
| Symptom | Common in Viral Tonsillitis | Common in Strep Throat | Key Differentiator |
|---|---|---|---|
| Sore Throat | Starts gradually, feels scratchy | Starts suddenly, intensely painful | The sudden onset and severe pain of strep are major red flags. |
| Cough/Runny Nose | Yes, very common. | Almost never. | The presence of cold symptoms strongly suggests a viral cause. |
| Fever | Low-grade or no fever. | Sudden, high fever (>101°F). | Strep often brings a spike in temperature. |
| Tonsil Appearance | Red and swollen. | Bright red, swollen, often with white pus streaks. | The classic "strep look" includes prominent white spots or pus. |
| Body Aches | Mild, if any. | Common and often severe. | Widespread aches and pains are more typical of strep throat. |
| Headache | Sometimes, usually mild. | Frequent and often intense. | A severe headache accompanying a sore throat points toward strep. |
| Nausea/Vomiting | Rare in adults. | Can occur, especially in children. | Stomach issues are more linked to strep, particularly in kids. |
While this table is a helpful guide, only a medical test can confirm a strep throat diagnosis.
Body-Wide Symptoms: Fever and Aches
How the rest of your body reacts also tells a big part of the story. The type of fever you have and other symptoms like headaches and body aches can be quite different between the two conditions.
Viral tonsillitis might come with a low-grade fever or none at all. If you do get one, it usually develops slowly along with your other cold symptoms.
Strep throat, in contrast, often hits you with a sudden, high fever, frequently climbing above 101°F (38.3°C). This is usually paired with a headache, body aches, and sometimes even nausea or vomiting, especially in children. When you have these intense, body-wide symptoms combined with a severe sore throat—but no cough—it paints a classic picture of strep.
How Doctors Confirm a Diagnosis: From Swabs to Certainty
When you’re staring at a raw, swollen throat, telling the difference between tonsillitis and strep throat based on looks alone is nearly impossible. That’s why doctors don’t just guess. To figure out what’s really going on—and make sure you get the right treatment—they turn to a couple of tried-and-true diagnostic tests.

It all starts with a simple throat swab. A healthcare provider uses a long, soft-tipped applicator to gently swipe the back of your throat and tonsils. It’s a bit uncomfortable and might make you gag for a second, but it’s over in a flash and is absolutely essential for getting a clear answer.
That one little sample holds the key to your diagnosis, as it can be used for two different tests.
The Rapid Antigen Detection Test (RADT)
More commonly known as the rapid strep test, this is the first line of defense in most clinics. It’s designed to quickly detect proteins (antigens) from the Group A Streptococcus bacteria right on the spot.
- How it Works: The swab is mixed with a solution that triggers a reaction if strep bacteria are present.
- Turnaround Time: You get an answer fast—usually within 5 to 10 minutes.
- Accuracy: It’s great for a quick confirmation, but it’s not perfect. Rapid tests can sometimes produce a false negative, meaning they might miss an active infection.
Thanks to its speed, a positive RADT means your doctor can get you started on antibiotics immediately. This helps you feel better sooner and cuts down the time you’re contagious. Getting a fast, accurate diagnosis is everything, and you can learn more about strep throat diagnosis and treatment to see all your options.
Key Insight: If a rapid test comes back positive, you can trust it. But a negative result doesn't always mean you're in the clear, especially if your symptoms are screaming "strep."
The Throat Culture: A More Definitive Answer
If the rapid test is negative but your doctor still has a strong suspicion of strep—especially for kids and teens who are more vulnerable to complications—they’ll often follow up with a throat culture. This test is the gold standard because of its high accuracy.
For a throat culture, another swab (or the original one) is sent off to a lab. There, technicians try to grow bacteria from the sample on a special plate. If Group A Streptococcus bacteria multiply, the diagnosis is confirmed.
- Turnaround Time: This one requires patience. Since the bacteria need time to grow, results take about 24 to 48 hours.
- Accuracy: A throat culture is far more sensitive than a rapid test and is excellent at catching infections the RADT might have missed.
This two-step diagnostic process is smart medicine. It ensures that a real bacterial infection doesn't go untreated, preventing serious issues like rheumatic fever. At the same time, it helps avoid prescribing unnecessary antibiotics for a viral infection. This careful, evidence-based approach is what finally settles the tonsillitis vs. strep throat debate.
Navigating Treatment Options: Antibiotics vs. Supportive Care
Once a doctor figures out if you have tonsillitis or strep throat, the road to recovery splits in two very different directions. The right treatment isn't a matter of preference—it’s dictated entirely by whether a virus or a bacteria is the culprit. Trying to throw antibiotics at a viral infection is like bringing a hammer to a software problem; it won’t work, and it can even cause bigger issues like antibiotic resistance down the line.
Getting this right is everything. For a virus, your own immune system is the hero. For a bacterial infection, your body needs backup from modern medicine to stop things from getting much worse.
The Essential Role of Antibiotics for Strep Throat
When a throat swab comes back positive for Group A Streptococcus, a course of antibiotics isn’t just a good idea—it’s non-negotiable. This isn’t just about feeling better faster. It’s about preventing some truly nasty complications. If left untreated, strep bacteria can lead to serious conditions like rheumatic fever, which can cause permanent heart damage, or kidney inflammation.
The most common prescriptions you'll see are:
- Penicillin or Amoxicillin: These are the go-to choices for a reason. They’re highly effective against strep bacteria and have a long track record of success.
- Alternative Antibiotics: If you have a penicillin allergy, don’t worry. Your doctor has other options, like cephalosporins or macrolides, that can get the job done.
Here’s the most important part: you absolutely must complete the entire 10-day course of antibiotics. Even if you feel a hundred times better after a day or two, stopping early is a huge mistake. It gives the toughest bacteria a chance to survive and come roaring back, potentially leading to a relapse or one of those serious complications we talked about.
Critical Takeaway: Antibiotics for strep throat do three crucial things: they shorten how long you're sick, they make you non-contagious within just 24 hours, and they are your single best defense against long-term health problems like rheumatic fever.
Supportive Care for Viral Tonsillitis
If your doctor confirms it's a virus, the game plan changes completely. Since antibiotics are useless against viruses, the focus shifts to supportive care. The goal here is simple: manage your symptoms and keep you as comfortable as possible while your immune system does the heavy lifting. This is all about rest and simple at-home remedies to soothe your throat and body.
Most of the time, viral tonsillitis clears up on its own within 7 to 10 days.
Effective At-Home Strategies
When it comes to viral tonsillitis, comfort is king. These tried-and-true strategies can make a real difference in how you feel:
- Stay Hydrated: Drink plenty of fluids. Warm liquids like herbal tea with a bit of honey or clear broth can feel amazing. On the other hand, cold liquids and popsicles can help numb a fiery throat.
- Gargle with Salt Water: It's an old-school remedy for a reason. Mix half a teaspoon of salt into eight ounces of warm water and gargle a few times a day. It’s surprisingly effective at reducing swelling and soothing irritation.
- Use Over-the-Counter Pain Relievers: Don’t be a hero. Medications like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are great for managing throat pain and knocking down a fever.
- Get Plenty of Rest: Your body is in a fight, and it needs all the energy it can get. Resting gives your immune system the fuel it needs to win.
- Soothe Your Throat: Keep some throat lozenges or hard candies handy. They’ll help keep your throat moist and provide some temporary relief from that scratchy feeling.
- Use a Humidifier: Running a humidifier, especially while you sleep, adds moisture to the air and can stop your throat from getting painfully dry.
Ultimately, the great tonsillitis vs. strep throat debate comes down to one simple truth: getting an accurate diagnosis is the first and most critical step toward feeling better. It ensures bacterial infections get the antibiotics they need while preventing the overuse of these powerful drugs for viral illnesses that just need a little time and care.
Recognizing When to Seek Medical Care
Figuring out if a sore throat is just a minor annoyance or a sign of something more serious can be tricky. While plenty of viral infections will clear up with rest and home remedies, certain symptoms are red flags telling you it's time to stop guessing and get a professional opinion.
Ignoring these warning signs can delay the right treatment, especially if a bacterial infection is the real culprit. The key is to pay attention to how severe your symptoms are and how they're evolving over time. A scratchy throat that shows up with a cough and runny nose? That usually points to a simple virus. But when the pain is intense and other specific symptoms join the party, you're dealing with a different situation.
Identifying Urgent Warning Signs
Some symptoms should never be ignored. If you or your child experience any of the following, it’s crucial to seek medical attention right away, as they could signal a severe infection or a complication that needs immediate intervention.
- Difficulty Breathing: Any trouble catching your breath or noisy breathing is a medical emergency.
- Trouble Swallowing: If you can't even swallow your own saliva or drink liquids, dehydration is a serious risk.
- A High, Persistent Fever: A fever that climbs above 103°F (39.4°C) and won’t come down with medication is a major concern.
- Stiff Neck or Trouble Opening Your Mouth: This could mean a more serious infection is spreading to the tissues nearby.
- A Spreading Rash: The appearance of a fine, sandpaper-like rash can be a sign of scarlet fever, a complication of strep throat.
These symptoms are way beyond the typical discomfort of a sore throat and demand an immediate evaluation to rule out anything serious.
This decision tree gives you a clear visual of how a sore throat is generally handled, showing the different paths for viral and bacterial causes.
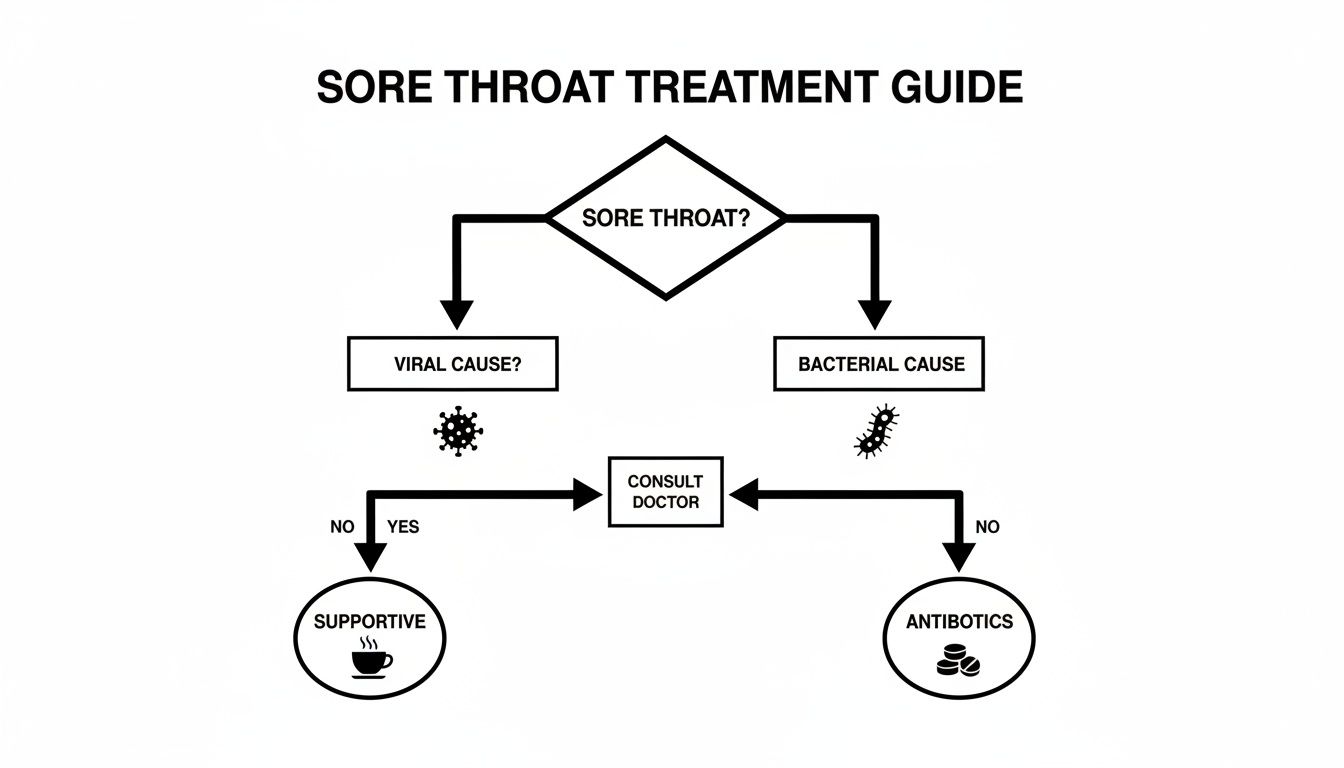
As the flowchart shows, while supportive care is the right call for viral infections, a confirmed case of strep throat needs targeted antibiotic treatment.
When a Professional Evaluation Is Best
Even if your symptoms aren't life-threatening, a doctor's input is still a smart move in many cases. Telling the difference between viral tonsillitis and bacterial strep throat on your own is nearly impossible without a proper test. Getting an official diagnosis is the only way to be sure you're getting the right care.
Key Insight: The main reason to see a doctor for a sore throat is to rule out strep. Since untreated strep can lead to serious complications like rheumatic fever, a proper diagnosis is your best defense.
You should definitely consider getting professional advice if your sore throat:
- Lasts longer than a week without getting any better.
- Comes with a sudden high fever and headache, but you don't have a cough.
- Includes swollen, tender lymph nodes in your neck.
- Shows visible white spots or pus on your tonsils.
For situations like these, getting a fast, accurate diagnosis is everything. When you need clear answers without the hassle of an in-person visit, platforms offering online urgent care are a convenient and effective solution. A quick consultation can get you a diagnosis and, if needed, a prescription sent straight to your pharmacy, helping you start the right treatment without delay.
Common Questions About Tonsillitis and Strep Throat
Even when you know the key differences between tonsillitis and strep throat, a few practical questions always seem to pop up. Knowing the real-world specifics on contagion, prevention, and whether it can come back helps you handle these common throat infections with confidence and keep your family healthy.
Here are some straight answers to the questions we hear most often.
How Long Are You Contagious?
The timeline for how long you're contagious really depends on whether the infection is viral or bacterial. It's a critical distinction for figuring out when it's safe to go back to work or send the kids to school.
For most cases of viral tonsillitis, you’re contagious as long as you have symptoms, which is usually about 7 to 10 days. The tricky part is that you can often start spreading it a day or two before you even feel sick.
Strep throat is a different beast entirely. Without medication, you can be highly contagious for up to three weeks. But this is where antibiotics make a huge difference, drastically shortening that window.
Key Insight: After you start antibiotics for strep throat, you're generally no longer considered contagious after a full 24 hours. This is exactly why it's so important to finish the whole prescription—it's not just for you, but to stop the spread to others.
Can I Get Strep Throat if I Don't Have Tonsils?
Yes, you absolutely can. While your tonsils are the prime real estate for a Group A Streptococcus infection, having them removed (a tonsillectomy) doesn't grant you immunity.
The bacteria can still set up shop in the back of your throat, a condition called strep pharyngitis. You’d get all the same classic symptoms—a sudden, miserable sore throat, fever, and pain when you swallow—and you would still need a full course of antibiotics to knock out the infection and prevent complications.
What Are the Risks of Untreated Strep Throat?
Letting strep throat run its course is a serious gamble. Sure, the sore throat might eventually fade on its own, but the underlying bacterial infection can spiral into some pretty significant health problems.
The most dangerous risk is acute rheumatic fever, a severe inflammatory condition that can surface weeks after the infection and cause permanent damage to your heart valves. Other potential complications include:
- Post-streptococcal glomerulonephritis: A serious kidney inflammation.
- Peritonsillar abscess: A painful pocket of pus that forms near where the tonsils were.
- Scarlet fever: A tell-tale rash that can show up alongside a strep infection.
This is precisely why getting a proper diagnosis and prompt antibiotic treatment is so non-negotiable in the tonsillitis vs. strep throat debate.
How Can I Prevent These Infections?
Preventing both conditions really boils down to good old-fashioned hygiene. Since viral and bacterial throat infections spread through respiratory droplets, your best defense is to break the chain of transmission. And if symptoms get severe or just won't quit, it's crucial to know when to get help; options like doctor at home services make getting a consultation incredibly convenient.
Here are the most effective strategies:
- Wash Your Hands Frequently: Use soap and water, especially after you cough or sneeze. It’s the simplest, most effective tool you have.
- Don't Share: Avoid sharing utensils, drinking glasses, or personal items like your toothbrush.
- Cover Your Mouth: Always cover your mouth and nose when you cough or sneeze.
- Swap Your Toothbrush: If you're diagnosed with strep, get a new toothbrush 24 hours after you start antibiotics to keep from reinfecting yourself.
When a sore throat strikes and you need answers fast, navigating your symptoms shouldn't be a source of stress. ChatWithDr offers same-day, text-based consultations with board-certified physicians for just $39.99. Get a diagnosis, a personalized treatment plan, and any necessary prescriptions sent to your pharmacy—all without leaving home. Start your confidential consultation now at https://chatwithdr.com.